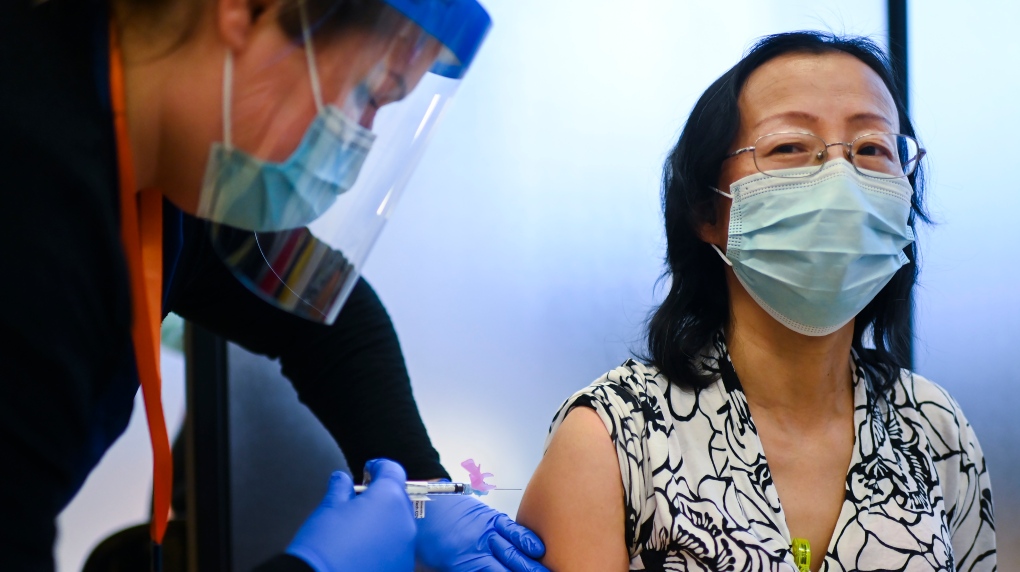
TORONTO -- The Ontario government will largely defer to the expertise of local public health units when it comes to decisions around who should receive the COVID-19 vaccine first among priority groups like health-care workers and long-term care residents.
Associate Medical Officer of Health Dr. Barbara Yaffe made the comment during a press conference on Wednesday as the province released the ethical framework that will guide its decision making in distributing COVID-19 vaccines.
She said that while the province has prioritized health-care workers, long-term care residents, home care patients with chronic conditions and First Nation communities as part of the first phase of its vaccine rollout, it will be leaving it up to local officials to determine the different subgroups that are “most at risk” within those broader classifications.
That means that decisions about which long-term care homes get the vaccine first and how health-care workers will be prioritized will largely be made at the local level in coordination with provincial officials.
“The first distribution of the Pfizer vaccine has been through a select number of hospitals due to the requirement to keep it at an extremely low temperature, however the vast amount of immunization (going forward) will be planned and coordinated through the local health units because the local health units have a very good sense of what is going on in their community,” Yaffe said. “So they will within the framework set by the province for prioritization be directing vaccine to the most risky within the priority groups.”
The Ontario government has said that it expects to be able to complete the vaccination of the initial priority groups sometime in March, at which point it will begin vaccinating the broader population.
Dr. Dirk Huyer, who is part of Ontario’s vaccine task force, said during Wednesday’s press conference that discussions are now underway about which groups will be prioritized in subsequent phases of the rollout and that “further clarification” could be provided in “the coming weeks.”
He said that as part of those discussions officials will look to prioritize those groups at higher risk of exposure, as well as those in critical roles.
The ethical framework specifically identifies “biological, social, geographical, and occupational factors” among those that should be considered in assessing risk.
It also says that the province must “actively work to reduce disparities in illness and death related to COVID-19, including disparities in the social determinants of health.”
“We want to protect those populations that are most at risk but not just due to biological factors but also due to social factors, to geological factors and occupational factors,” bioethicist Dr. Maxwell Smith, who also sits on the vaccine task force, told reporters. “It is not terribly straight forward identifying the exact populations that those point to but absolutely those are the sorts of considerations that the ethical framework requires us to think through.”
These are the six overarching principals included in Ontario’s ethical framework:
- Minimize harms and maximize benefits, to reduce overall illness and death related to COVID-19, protect those at greatest risk of serious illness and death due to biological, social, geographical and occupational factors, protect critical infrastructure, and promote social and economic well-being;
- Equity in the distribution of vaccines without bias or discrimination, to reduce disparities in illness and death related to COVID-19, and ensuring benefits for groups experiencing greater burdens from the COVID-19 pandemic;
- Fairness, to ensure that every individual within equally prioritized groups has the same opportunity to be vaccinated, and to ensure inclusive, consistent processes that are tailored to unique needs of Ontario's many and varied communities when making decisions about vaccine prioritization;
- Transparency, to ensure the principles and rationale, decision-making processes and plans for COVID-19 prioritization are clear, understandable and communicated to the public;
- Legitimacy, making decisions based on the best available scientific evidence, shared values and input from affected parties including those historically underrepresented, to ensure decisions have the intended impact, and to include participation of affected parties in the creation and review of decisions and decision-making processes; and
- Public trust, to ensure decisions and decision-making processes are informed by these principles to advance confidence and trust in Ontario's COVID-19 immunization program.