How Ontario's 'breakthrough' COVID-19 cases show that vaccines work
Since the province began vaccinating some of the most vulnerable populations in Ontario, COVID-19 trends have dropped dramatically compared to the peak of the third wave.
While even fully vaccinated individuals can still contract the virus and end up in a hospital, experts say those incidents will become fewer and further between as Ontario’s rollout continues.
An infectious diseases specialist in Hamilton is planning on studying just how many lives have been, and will be, saved as a result of a vaccination.
"(I'll) go through the Ontario data that's out there and just try to see the 'what if' scenarios, if we didn't vaccinate in our third wave, if we didn't vaccinate long term care," Dr. Zain Chagla, a physician at St. Joseph's Hospital, said. "There probably would be 1,500 (or) 2,000 more deaths, but we never will count those."
Chagla says he wants to reframe how people think about reported COVID-19 cases in vaccinated individuals.
This comes after a COVID-19 outbreak this week at Toronto Western Hospital, which ended up impacting some patients and staff who had either one or both doses of a COVID-19 vaccine.
So far, four staff members and four patients have been impacted, but all of them are reporting mild or asymptomatic cases.
"We would love to have no COVID-19, but if it is a mild illness, then it doesn't really affect that person's hospitalization and they're discharged home appropriately, then the vaccines are doing what they're supposed to be doing," Chagla said. "Many of these headlines don't emphasize the number of people that these vaccines either prevented transmission for... or other people that that it prevented significant medical illness, ICU stays, or death from."
Much of the data Chagla will focus on comes from Public Health Ontario, which details how many breakthrough cases—infections identified in people who have received two doses of a COVID-19 vaccine at least seven days prior to infection or one dose 14 days prior—the province has recorded and what the severity of each case was.
The latest available data ranges from December 14, 2020 to June 12, 2021, and shows how much of an impact vaccines are having on seniors in Ontario.
During that time period, there has only been one person aged 80 or older who has ended up in a intensive care unit (ICU) after being fully vaccinated, compared to 303 ICU patients in that same age group who were unvaccinated.
"Of the almost 9.4 million vaccinated individuals only 0.15 (per cent)... became infected when they were partially vaccinated and only 0.02 (per cent)... became infected when they were fully vaccinated," Public Health Ontario's report states.
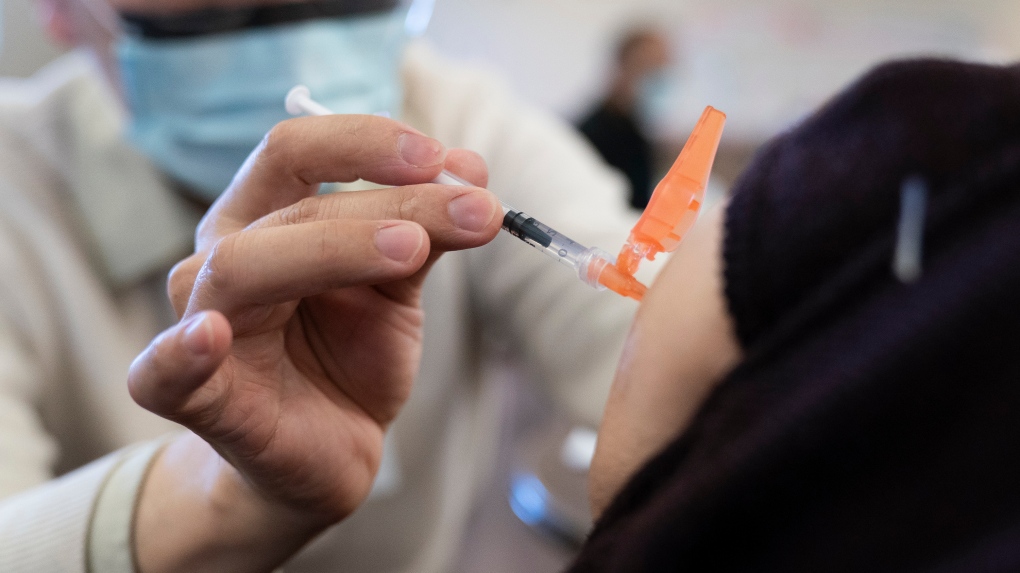 Dr. E. Kwok administers a COVID-19 vaccine to a recipient at a vaccination clinic run by Vancouver Coastal Health, in Richmond, B.C., Saturday, April 10, 2021. THE CANADIAN PRESS/Jonathan Hayward
Dr. E. Kwok administers a COVID-19 vaccine to a recipient at a vaccination clinic run by Vancouver Coastal Health, in Richmond, B.C., Saturday, April 10, 2021. THE CANADIAN PRESS/Jonathan Hayward
Dr. Ruchi Murthy is an infectious diseases specialist at Queensway Carleton Hospital in Ottawa and she points out it's far less common to become infected with COVID-19 after vaccination—and even more rare to experience a severe outcome if you do get sick.
"I think we need to take a step back and appreciate what the big picture goal was for these vaccines," Murthy said. "The goal was to reduce community transmission, it was to reduce numbers in hospitals, and it was to try to reduce severe illness and death. So far, what we've seen locally is that we're starting to see trends that all of this is happening with vaccines."
Murthy says there will never be a perfect solution to eradicating COVID-19 in the short-term, but if we can manage how sick people get and how strong the virus is, then it becomes a lot easier to live with.
"Certainly, my heart does go out to those that have still become unwell and had illness or death related to COVID infection despite vaccinations," Murthy said.
"But if you look at the vast majority of the numbers, we are seeing some wins with the... uptake of vaccines that Canadians have participated in. We're not quite out of the woods yet, though. We know that with the rising Delta variant that we do need two doses to best protect ourselves... and it's something that we all need to participate in still to get those shots in arms."
HOSPITALS STRUGGLE WITH BACKLOG AS COVID-19 PATIENTS DECLINE
As the number of COVID-19 patients in Ontario hospitals continues to decline, the head of general surgery at Sunnybrook Hospital is warning of a “huge backlog.”
"Right now, we're full tilt," Dr. Shady Ashamalla said. "There's this huge backlog, and we're able to, as soon as we're able to decompress, and there's space, then we really crank up what we do."
The pandemic has created a backlog of an estimated 15.9 million medical procedures, according to the Ontario Medical Association.
 A health-care worker wearing PPE transports a patient in the dialysis unit at the Humber River Hospital during the COVID-19 pandemic in Toronto on Wednesday, December 9, 2020. THE CANADIAN PRESS/Nathan Denette
A health-care worker wearing PPE transports a patient in the dialysis unit at the Humber River Hospital during the COVID-19 pandemic in Toronto on Wednesday, December 9, 2020. THE CANADIAN PRESS/Nathan Denette
Ashamalla says that catching up on those procedures will be a top priority through the summer and fall, there are other added complications from the pandemic, especially for cancer patients.
"We know that there was... quite a long period of time where screening for cancers really decreased across the province, that in of itself will have an impact that we don't necessarily know yet," Ashamalla said.
"We have diagnosed far less cancers this year than years past... and the only difference is really the fact that we didn't screen, which means there are many, many patients out there whose screening has been delayed, who are carrying some disease burden, who don't know it yet, who have yet to come to medical attention."
On top of that, Ashamalla says, some patients will have had a change in prognosis through the pandemic due to health-care system delays, and the effects of that won't show up until further down the road.
But for now, things are getting back on track.
"I'd like to say, with a fair bit of confidence that the worst is absolutely behind us. I know that there's a lot of anxiety around different variants, and there's a lot of anxiety around the impact and things that might happen again, in the future.... I will say that we are in a very good place. And I do believe we're on the other side of this."
CTVNews.ca Top Stories

Budget 2024 prioritizes housing while taxing highest earners, deficit projected at $39.8B
In an effort to level the playing field for young people, in the 2024 federal budget, the government is targeting Canada's highest earners with new taxes in order to help offset billions in new spending to enhance the country's housing supply and social supports.
BUDGET 2024 Feds cutting 5,000 public service jobs, looking to turn underused buildings into housing
Five thousand public service jobs will be cut over the next four years, while underused federal office buildings, Canada Post properties and the National Defence Medical Centre in Ottawa could be turned into new housing units, as the federal government looks to find billions of dollars in savings and boost the country's housing portfolio.
Some of the winners and losers in the 2024 federal budget
With a variety of fiscal and policy measures announced in the federal budget, winners include small businesses and fintech companies while losers include the tobacco industry and Canadian pension funds.
From housing initiatives to a disability benefit, how the federal budget impacts you
From plans to boost new housing stock, encourage small businesses, and increase taxes on Canada’s top-earners, CTVNews.ca has sifted through the 416-page budget to find out what will make the biggest difference to your pocketbook.
Police to announce arrests in Toronto Pearson airport gold heist
Police say that arrests have been made in connection with a $20-million gold heist at Toronto Pearson International Airport one year ago.
Teen hockey players arrested for sexual assault following hazing incident: Manitoba RCMP
Three teenagers were arrested in connection with a pair of alleged hazing incidents on a Manitoba hockey team, police say.
'I Google': Why phonebooks are becoming obsolete
Phonebooks have been in circulation since the 19th century. These days, in this high-tech digital world, if someone needs a phone number, 'I Google,' said Bridgewater, N.S., resident Wayne Desouza.
Liberals aim to hit the brakes on car theft with new criminal offences
The Liberals are proposing new charges for the use of violence while stealing a vehicle and for links to organized crime, as well as laundering money for the benefit of a criminal organization.
BUDGET 2024 Ottawa police get $50 million to boost security around Parliamentary Precinct
The Ottawa Police Service will receive $50 million in new federal funding over the next five years to "enhance security" around the Parliamentary Precinct.































