Half of Ontario opioid deaths interacted with health-care system the month before: study
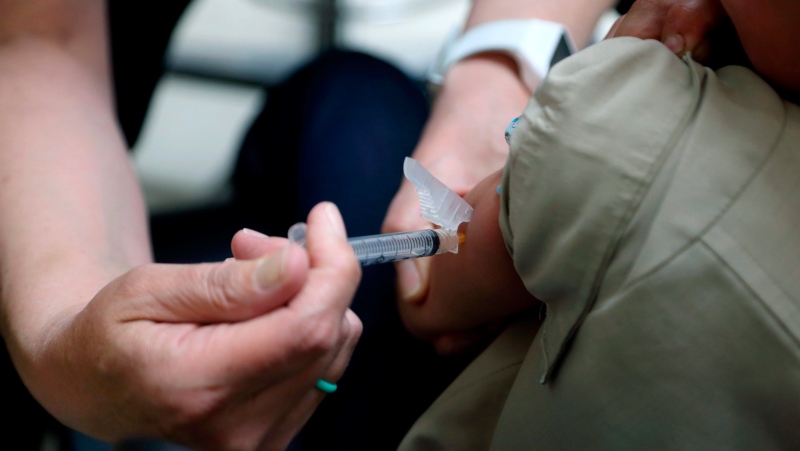
 Prescription pills containing oxycodone and acetaminophen are shown on June 20, 2012. THE CANADIAN PRESS/Graeme Roy
Prescription pills containing oxycodone and acetaminophen are shown on June 20, 2012. THE CANADIAN PRESS/Graeme Roy
Half of Ontarians who died of an opioid overdose in the early stages of the pandemic had interacted with the health-care system in the month before their deaths, a new report shows.
And one in four had seen a doctor, gone to an emergency department or been discharged from hospital just a week prior, the research shows.
"That represents such an important missed opportunity for us to make sure that our health-care system is serving the needs of people who use drugs and helping connect them to the services that they need to help prevent these fatal overdoses," said Dr. Tara Gomes, an epidemiologist with Unity Health and investigator with the Ontario Drug Policy Research Network who co-authored the study.
The report, titled "Patterns of Medication and Healthcare Use among People who Died of an Opioid-Related Toxicity during the COVID-19 Pandemic in Ontario," was released Tuesday by Unity Health and the Ontario Drug Policy Research Network. Public Health Ontario, the chief coroner's office and ICES, the non-profit health research organization, contributed to the report.
The authors are calling for a safer drug supply, expanded access to low-barrier treatment in health-care settings, affordable, supportive housing as well as more harm-reduction services and supervised consumption sites, especially outside cities.
"The loss of lives due to opioid toxicity in Ontario has only deepened during the COVID-19 pandemic," said Dr. Dirk Huyer, the Chief Coroner for Ontario, in a statement.
"Understanding how people interact with healthcare providers, support systems, and harm reduction services will help develop policies aimed at preventing further opioid-related deaths."
The vast majority of deaths recorded between March and December 2020 -- 89 per cent -- are linked to non-prescription opioids, almost exclusively fentanyl, the report found.
Gomes said two in three deaths occurred in those with evidence of an opioid use disorder. That means about one third of people had no evidence of a substance use disorder.
"It's likely that a large number of those people are people who are just occasionally using drugs," she said.
"And they might actually be a population at higher risk of overdose from this really unpredictable drug supply because they haven't developed the same level of tolerance to these really potent drugs."
The research follows up on the group's work published in May, which showed fatal opioid overdoses were up more than 75 per cent in Ontario from March to December 2020 compared to the same timeframe the year before.
There were 2,050 people who died of an opioid-related overdose in about 10 months, compared to 1,162 from March to December 2019.
The researchers were able to link the vast majority of those deaths to other health-care data in an effort to better understand some of the circumstances.
The increasingly volatile drug supply appears to be connected to the surge, Gomes said.
"Though the role of prescription opioids has historically been focused on as the major contributor to the overdose crisis, the report shows that the unregulated drug supply is primarily responsible for fatal overdoses, with deaths predominantly driven by fentanyl," the report said.
The researchers detected a five-fold increase in non-pharmaceutical benzodiazepines in fatal opioid overdoses during the pandemic.
"It's not that people are getting prescribed anti-anxiety medication, but that the unregulated drug supply is really being contaminated by benzodiazepines," Gomes said.
The addition of benzodiazepines has further complicated the response to an overdose and subsequent treatment, she said.
"We're hearing people who are so highly sedated for the benzodiazepines in the drug supply that they can't be roused for hours and hours at a time even after administering Naloxone because that only reverses the opioid effect," Gomes said.
She said opioids mixed with benzodiazepines have been shown "to increase respiratory depression and sedation so it can make you more likely to have an overdose and a serious overdose because you're still heavily sedated and your breathing is you know, slowed even further."
The researchers also found that, when population is factored in, the opioid overdose death rate was nearly three times higher in northern Ontario compared to southern Ontario.
Meanwhile, the researchers dug into further understanding why the opioid crisis was hitting the homeless much harder than other populations, after their previous report found one in six people who died from an opioid overdose during the pandemic did not have a home.
The researchers found that population was interacting with the health-care system in similar rates as the rest of the population in the days and weeks before their deaths, but was much more likely to seek help from an emergency department than outpatient care, like a visit to a family doctor.
Gomes said they are seeing a high degree of mental health diagnoses among the homeless who died of an opioid overdose.
"Given the increasing rates of overdose among people experiencing homelessness during the pandemic, the scale-up of supervised consumption services in shelter settings and easily accessible treatment options is warranted," the researchers wrote.
This report by The Canadian Press was first published Jan. 18, 2022.
CTVNews.ca Top Stories
Doctors say capital gains tax changes will jeopardize their retirement. Is that true?
The Canadian Medical Association asserts the Liberals' proposed changes to capital gains taxation will put doctors' retirement savings in jeopardy, but some financial experts insist incorporated professionals are not as doomed as they say they are.
Something in the water? Canadian family latest to spot elusive 'Loch Ness Monster'
For centuries, people have wondered what, if anything, might be lurking beneath the surface of Loch Ness in Scotland. When Canadian couple Parry Malm and Shannon Wiseman visited the Scottish highlands earlier this month with their two children, they didn’t expect to become part of the mystery.
Fair in Ontario, flurries in Labrador: Weather systems make for an erratic spring
It's no secret that spring can be a tumultuous time for Canadian weather, and as an unseasonably mild El Nino winter gives way to summer, there's bound to be a few swings in temperature that seem out of the ordinary. From Ontario to the Atlantic, though, this week is about to feel a little erratic.
What do weight loss drugs mean for a diet industry built on eating less and exercising more?
Recent injected drugs like Wegovy and its predecessor, the diabetes medication Ozempic, are reshaping the health and fitness industries.
He replaced Mickey Mantle. Now baseball's oldest living major leaguer is turning 100
The oldest living former major leaguer, Art Schallock turns 100 on Thursday and is being celebrated in the Bay Area and beyond as the milestone approaches.
What a urologist wants you to know about male infertility
When opposite sex couples are trying and failing to get pregnant, the attention often focuses on the woman. That’s not always the case.
'It was instant karma': Viral video captures failed theft attempt in Nanaimo, B.C.
Mounties in Nanaimo, B.C., say two late-night revellers are lucky their allegedly drunken antics weren't reported to police after security cameras captured the men trying to steal a heavy sign from a downtown business.
Bank of Canada officials split on when to start cutting interest rates
Members of the Bank of Canada's governing council were split on how long the central bank should wait before it starts cutting interest rates when they met earlier this month.
Made-in-Newfoundland vodka claims top prize at worldwide competition
A Newfoundland-made vodka has been named one of the world’s best by judges at this year’s World Vodka Awards.